Nail fungus, medically known as onychomycosis, is a condition that plagues millions worldwide, turning what seems like a minor nuisance into a frustratingly persistent problem. If you’ve ever dealt with discolored, thickened, or brittle nails that just won’t clear up despite your best efforts, you’re not alone. But why is nail fungus so persistent? What makes treating it such a challenge? In this comprehensive guide, we’ll dive into the science behind nail fungus persistence, explore the obstacles to effective treatment, and offer insights into overcoming this stubborn condition.
Table of Contents
ToggleWhat Causes Nail Fungus Persistence?
Nail fungus doesn’t just appear out of nowhere—it thrives due to a combination of environmental, biological, and lifestyle factors. Understanding what causes nail fungus persistence is the first step to tackling it effectively.
Fungi, particularly dermatophytes like Trichophyton rubrum, love warm, moist environments—think sweaty socks, damp shoes, or public pools. Once they invade the nail bed or nail plate, they dig in deep, feeding on keratin, the protein that makes up your nails. This isn’t a surface-level infection; it’s a tenacious intruder that embeds itself where it’s hard to reach. Add to that poor hygiene, frequent moisture exposure, or a weakened immune system, and you’ve got a recipe for a persistent fungal takeover.
But it’s not just external factors. The nail itself acts as a fortress, shielding the fungus from quick eradication. Its slow growth rate—fingernails take 4-6 months to fully regrow, toenails up to 12-18 months—means the infection has plenty of time to settle in. This slow turnover is a key reason why nail fungus persistence frustrates so many.
The Biology of Stubborn Nail Infections
To grasp why treating persistent nail fungus is such a battle, let’s look at the biology behind it. Fungi aren’t like bacteria—they’re tough, resilient organisms with survival strategies that make them hard to kill.
Fungal Resilience
Fungi produce spores, microscopic seeds that can lie dormant and resist harsh conditions, including some antifungal treatments. These spores can reactivate once the environment becomes favorable again, making recurrence a constant threat. This durability is a major contributor to stubborn nail infections.
Nail Structure as a Barrier
The nail plate is a hard, compact layer of keratin that protects the nail bed—but it also protects the fungus. Antifungal creams and solutions struggle to penetrate this barrier, leaving the infection safe beneath the surface. Even oral medications, which attack from within, face challenges reaching adequate concentrations in the nail.
Biofilm Formation
Some fungi form biofilms—protective slime layers that shield them from drugs and the immune system. Research from 2023 shows that biofilms in nail infections are a growing concern, adding another layer to the challenges of nail fungus treatment. This biological armor explains why even aggressive therapies sometimes fall short.
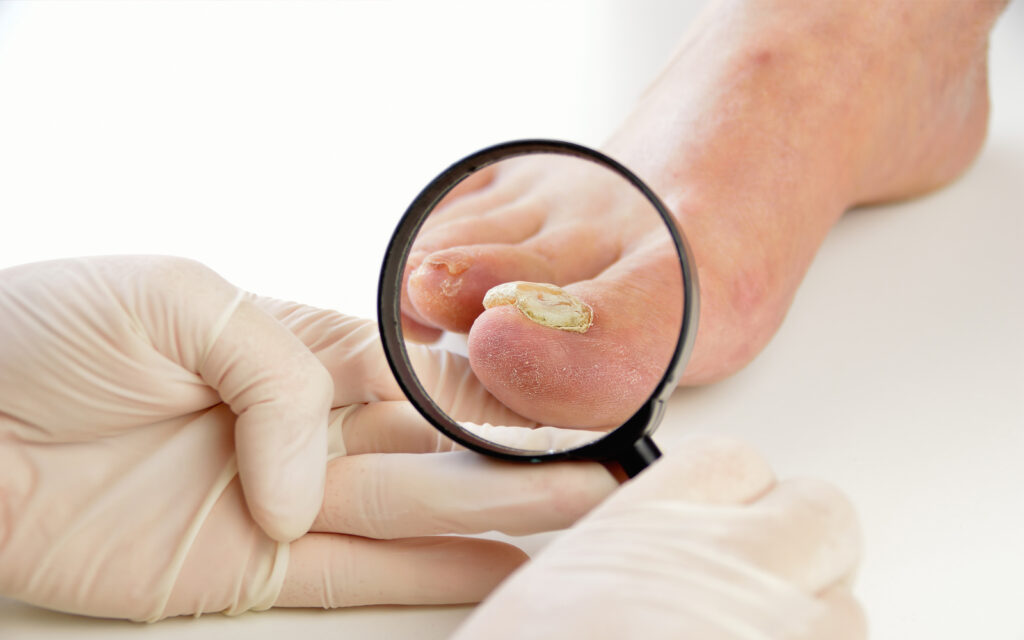
Challenges of Nail Fungus Treatment: Why It’s So Tough
Treating nail fungus isn’t as simple as applying a cream and calling it a day. Several obstacles make it a long, uphill fight.
Slow Nail Growth
As mentioned, nails grow slowly—especially toenails, where fungus is most common. This means any treatment must persist long enough to outlast the infection as the nail gradually replaces itself. Miss a dose or stop too early, and the fungus regroups, undoing your progress.
Drug Penetration Issues
Topical treatments, like antifungal lacquers, face the nail’s natural barrier. Studies show that only a small percentage of the active ingredient reaches the nail bed, where the fungus lives. Oral antifungals (e.g., terbinafine or itraconazole) are more effective but require months of use and aren’t always an option due to side effects like liver strain.
Resistance to Treatment
Fungal strains can develop resistance, especially with improper use of antifungals—like stopping treatment prematurely or using over-the-counter remedies inconsistently. This resistance is a growing challenge, with 2024 data suggesting that up to 20% of cases now involve harder-to-treat strains.
Underlying Health Factors
Conditions like diabetes, poor circulation, or a compromised immune system (e.g., from chemotherapy) make treating persistent nail fungus even tougher. These factors impair the body’s ability to fight the infection naturally, leaving treatments to do all the heavy lifting.
Misdiagnosis and Delayed Action
Not every nail problem is fungal—psoriasis or trauma can mimic onychomycosis. Misdiagnosis delays proper care, letting the fungus dig deeper. Even when correctly identified, many delay treatment, thinking it’s “just cosmetic,” only to face a more entrenched infection later.
Common Nail Fungus Remedies and Their Limits
From drugstore solutions to prescription meds, here’s a look at popular nail fungus remedies and why they often fall short in tackling stubborn nail infections.
Over-the-Counter Topicals
Products like antifungal creams or tea tree oil are affordable and accessible, but their penetration is limited. They might work for mild, early-stage infections, but for deep-seated fungus, they’re like throwing water on a grease fire—ineffective and temporary.
Prescription Medications
Oral antifungals like terbinafine boast cure rates of 60-80%, but they require 3-6 months of daily use and regular liver monitoring. Topical prescriptions (e.g., ciclopirox) are safer but less effective, with success rates below 50%. Both face the challenge of nail fungus persistence if not used diligently.
Home Remedies
Vinegar soaks, Vicks VapoRub, and essential oils are popular DIY fixes, but evidence is anecdotal at best. A 2023 study found vinegar might inhibit fungal growth in a lab, but real-world results are inconsistent. These remedies lack the potency to address fungal nail treatment obstacles head-on.
Laser Therapy
Emerging laser treatments zap fungi with light energy, offering hope for resistant cases. Success rates hover around 50-70%, but costs (often $500-$1,000 per session) and limited long-term data as of 2025 make it a gamble for many.
Overcoming Fungal Nail Treatment Obstacles
So, how do you beat nail fungus persistence? It takes a multi-pronged approach combining medical intervention, lifestyle changes, and patience.
Consult a Specialist
A dermatologist or podiatrist can confirm the diagnosis with a nail clipping test and tailor a treatment plan. For severe cases, they might combine oral and topical therapies to attack from multiple angles.
Commit to Consistency
Whether it’s applying a lacquer daily or taking pills for months, sticking to the regimen is non-negotiable. Stopping early invites recurrence—think of it as letting a weed regrow after pulling half the root.
Improve Nail Hygiene
Keep nails dry and trimmed, avoid tight shoes, and rotate footwear to prevent moisture buildup. Antifungal powders or sprays can help maintain a hostile environment for fungi.
Explore Advanced Options
Hydro jetting isn’t just for drains—similar high-tech principles inspire treatments like laser therapy or photodynamic therapy (using light-activated drugs). These are worth discussing with a doctor if standard treatments fail.
Address Underlying Risks
Manage diabetes, boost circulation with exercise, or strengthen immunity through diet. These steps don’t cure the fungus directly but make your body a tougher battlefield for it.
FAQ
1. Why does nail fungus keep coming back after treatment?
Recurrence happens due to fungal spores, incomplete treatment, or re-exposure to moist environments. Consistent care and hygiene are key to preventing it.
2. How long does it take to treat persistent nail fungus?
Depending on severity, it can take 6-18 months for a nail to fully clear as it grows out. Patience is crucial.
3. Are home remedies effective for stubborn nail infections?
They may help early on but lack the strength to penetrate deep infections. Professional options are more reliable.
4. Can nail fungus spread to other parts of the body?
Yes, if untreated, it can spread to other nails, skin, or even internally in rare cases, especially if immunity is low.
5. Is laser therapy worth it for nail fungus persistence?
It shows promise for resistant cases, but costs and variable results mean it’s not a first-line choice yet.
It is important for people considering skin tag removal in plano , laser hair removal in plano ,microneedling in plano, Hydrafacial in plano, Microdermabrasion plano, Laser electrolysis plano, Nail Fungus plano, Rosacea Treatment in plano, Spider Vein Removal plano, Wrinkle Reduction in plano, Botox in plano, Hifu in plano,Oxygeno Facial in Plano to undergo a full consultation with a qualified doctor or cosmetologist – Aesthetician Nasrin, – to assess their suitability for this procedure and discuss their .
No comment yet, add your voice below!